Eating a diet filled with animal products can destroy the microbiota faster than taking antibiotics.
Search online for “Crohn’s Disease and Diet” or “Ulcerative Colitis and Diet” and the top results are a jumble of conflicting advice, as seen below and in my video to prevent inflammatory bowel disease.
What do science say? A systematic review of the medical literature on dietary intake and risk of developing inflammatory bowel disease has found that while Crohn’s disease is associated with fat and meat intake, dietary fiber and fruit appear to be protective. The same associations are ulcerative colitis, other major inflammatory bowel diseases, namely increased risk of fat and meat, and protection with vegetable intake.
Why are meat consumers at about 50% higher risk of inflammatory bowel disease, according to this meta-analysis of nine separate studies? One possibility is that meat may be the bacterial vehicle that plays a role in the development of such diseases. For example, meat contains “a huge amount of Yersinia.” Although the antibiotic residues in the meat itself can theoretically induce our microbiota, Yersinia is a so-called psychotropic bacteria that can grow at refrigerator temperatures and are known to be significantly associated with inflammatory bowel disease (IBD). This supports the concept that Yersinia infection may be a trigger for chronic IBD.
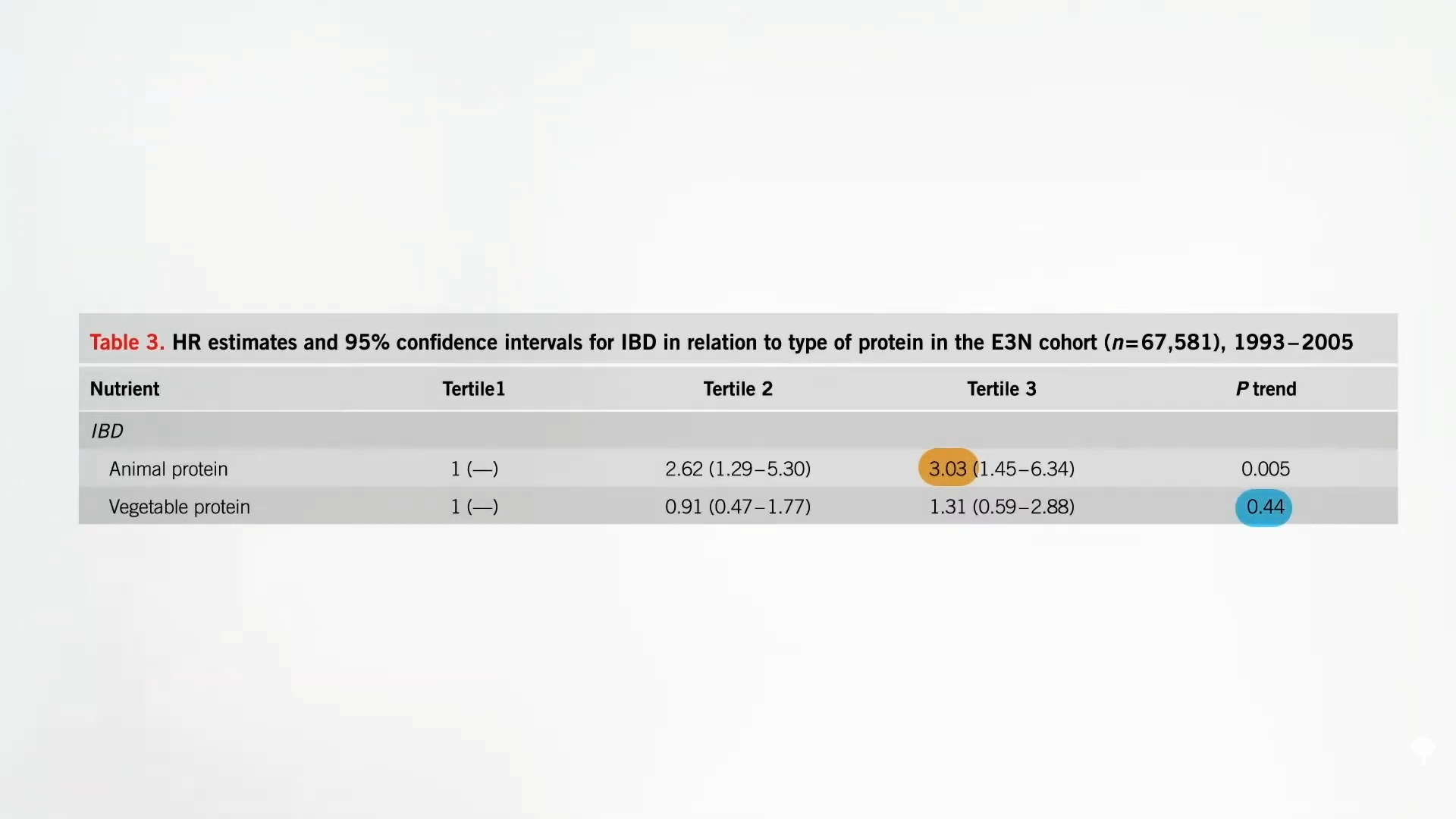
Animal proteins are associated with triple risk of inflammatory bowel disease, but plant proteins are not, as shown below and at 1:39 in my video. why? One reason is that animal proteins can lead to the formation of toxic bacterial end products, such as hydrogen sulfide, a rotten egg gas. Hydrogen sulfide is not just “one of the major malodras compounds in human Flatus.” It is “venoms associated with ulcerative colitis.” So, if you’re on a meaty, low-carb diet, we’re not talking about “Marodos proctitis,” but we’re at an increased risk of irritable bowel syndrome, inflammatory bowel syndrome (ulcerative colitis), and ultimately colorectal cancer.

Hydrogen sulfide in the colon come From sulfur-containing amino acids, such as methionine, concentrated in animal proteins. Also, sulfites have been added as preservatives for some non-organic wines and non-organic dried fruits, but sulfur-containing amino acids may be the more important of the two. The researcher I gave it Those increasing the amount of meat have increased their fecal sulfide, as seen here at my 2:37. video.
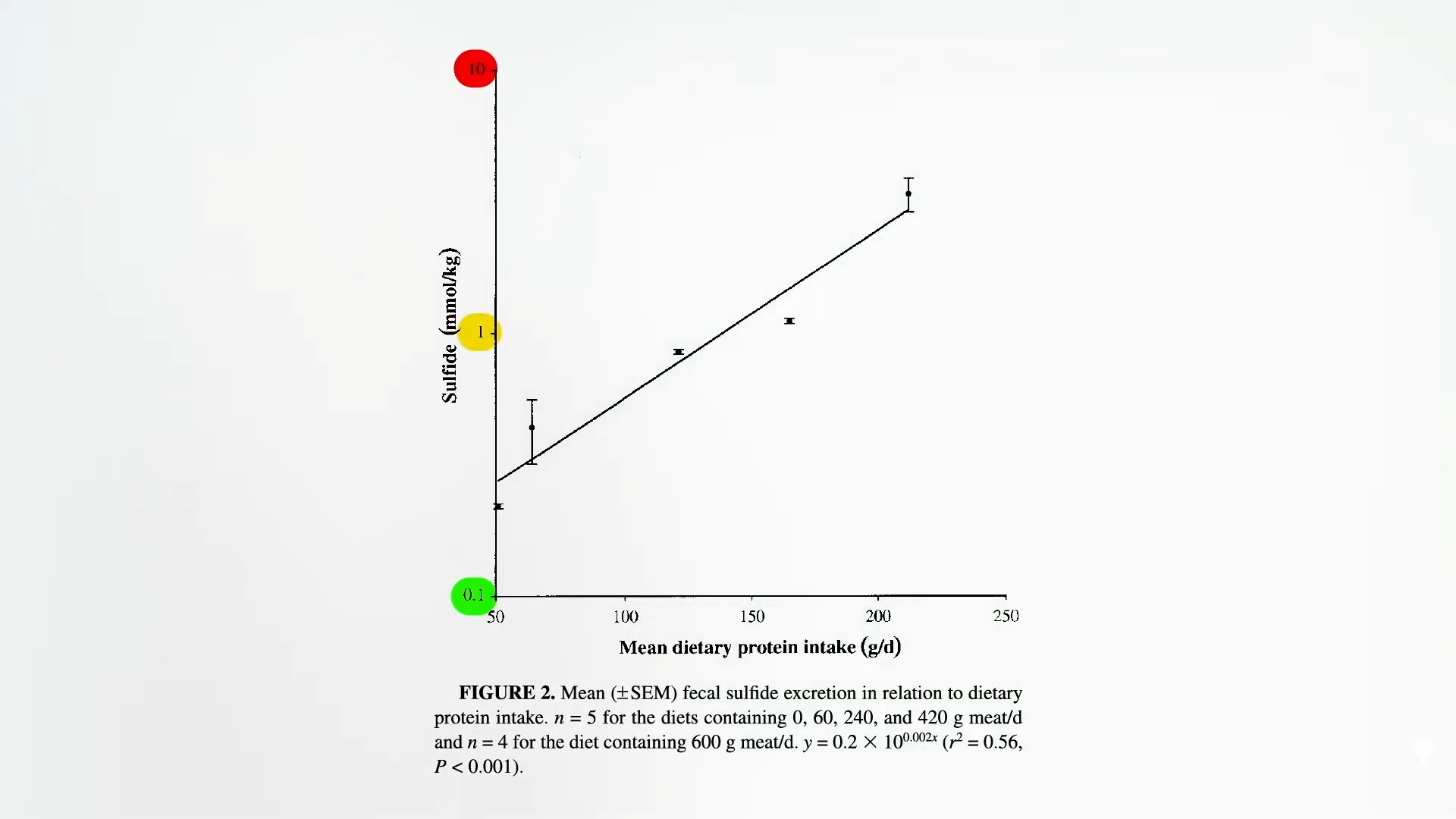
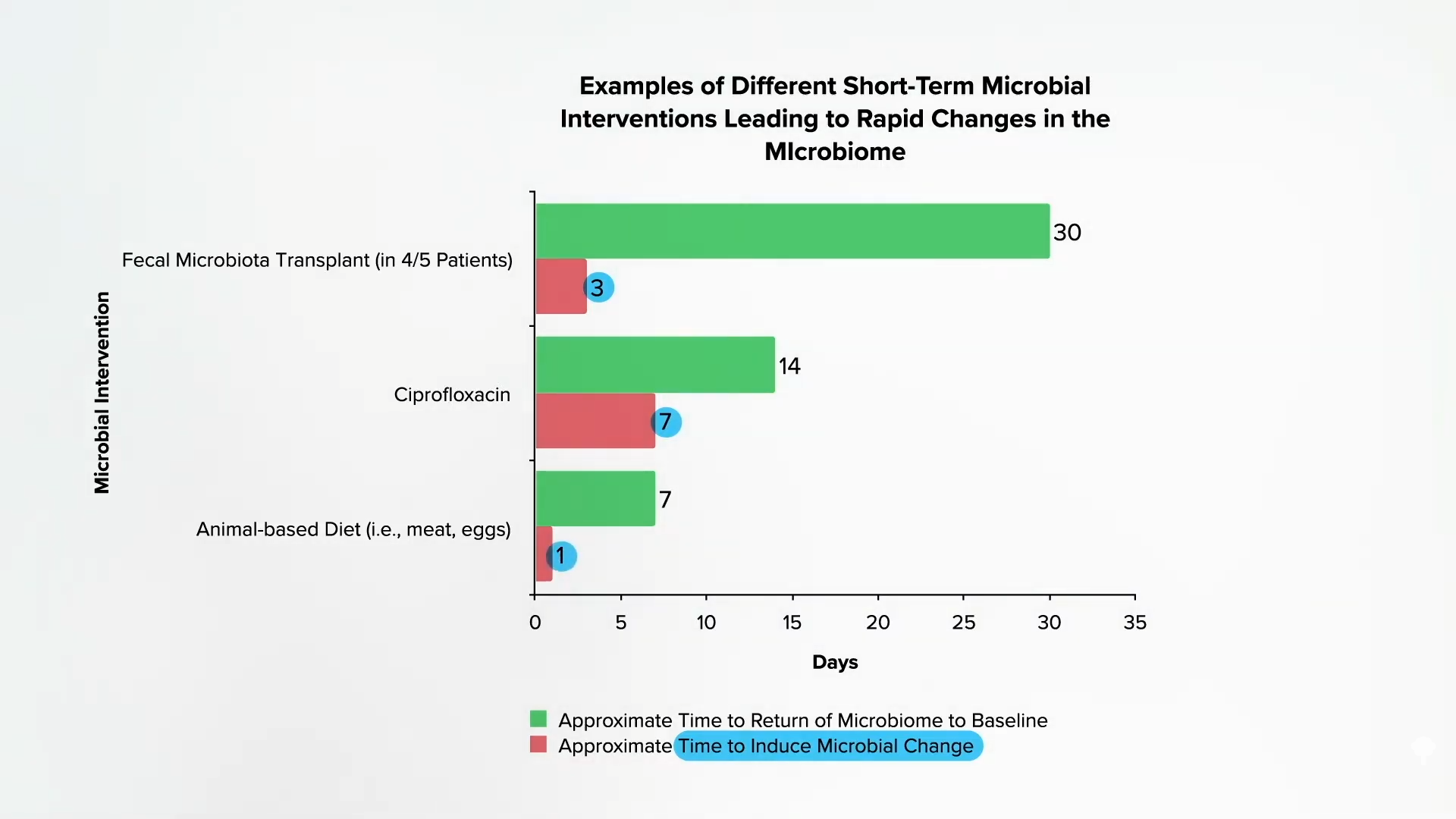
Certain bacteria, such as Biophilia wadsworthia, can take this sulfur, which ends up in our colon and produces hydrogen sulfide. Eating a diet based on animal products stuffed with meat, eggs and dairy products can especially increase the growth of this bacteria. People are underestimating the dramatic effects that diet can have on our gut bacteria. As shown at 3:12 in my video, when people are given a fecal transplant, it can take three days for the microbiota to shift. Taking powerful antibiotics like Cipro can take a week. However, if we start eating a heavy meal with meat and eggs within a day, our microbiota can change. The bad bacterial mechanisms that stir hydrogen sulfide have more than doubled, consistent with the idea that “diet-induced changes in the gut microbiota (flora) may contribute to the development of inflammatory bowel disease.” In other words, the increase in colonic sulfur compounds when we eat meat “is not only of interest in the field of squamous disease” – human fart research – “However, it may be important in the pathogenesis of ulcerative colitis.”
Doctor’s notes:
This is the first in a three-part video series. Stay tuned for the perfect diet for the treatment of ulcerative colitis and the perfect diet for the treatment of Crohn’s disease.





